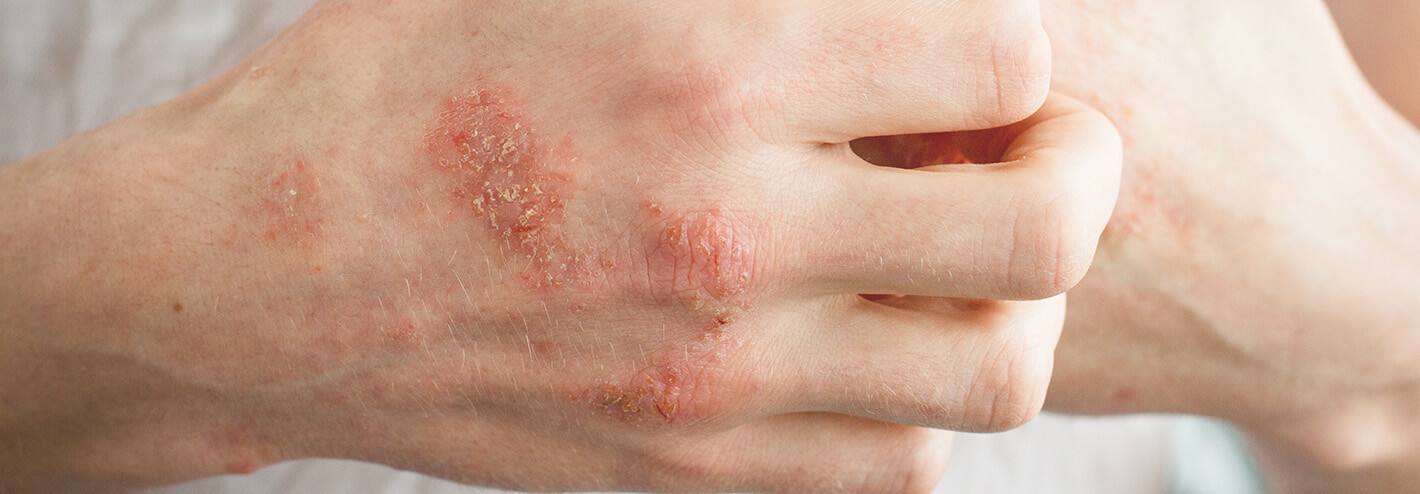
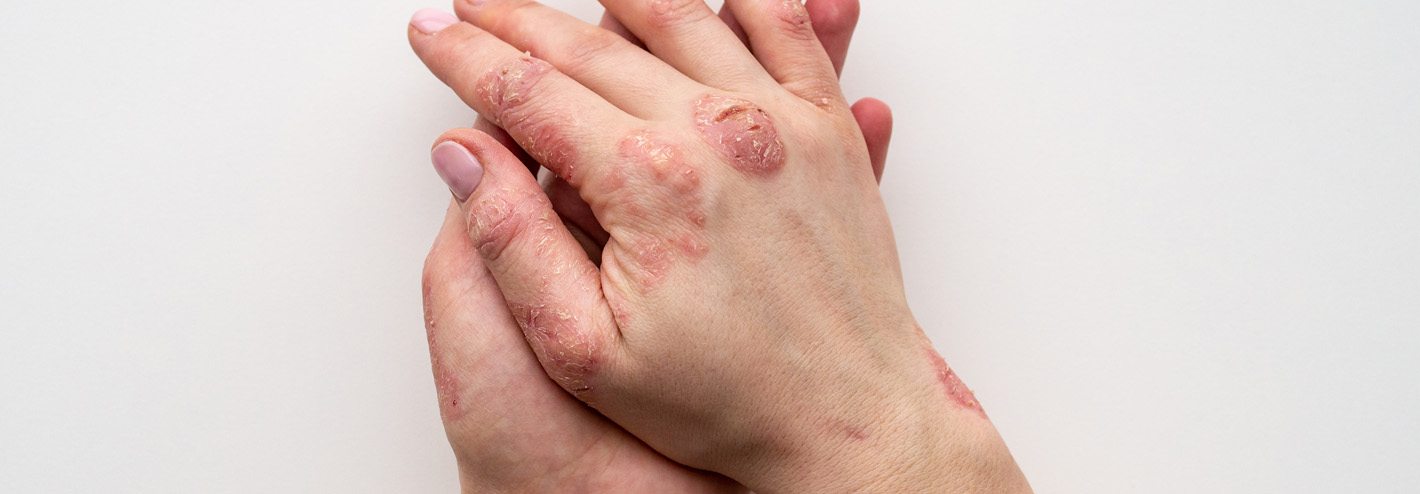
What causes atopic dermatitis?
Atopic dermatitis is a non-infectious condition, so cannot be passed
between people. We remain unclear about the specific cause of atopic
dermatitis, but know of multiple factors related to the condition.
Patients usually have a pre-existing susceptibility to developing the
condition, which is then triggered by factors within their environment.
Individuals can be susceptible to developing atopic dermatitis due to
genetic factors that influence either their skin barrier, immune response,
or both:
Skin barrier: changes to the filaggrin gene alter the
healthy skin barrier, making patients more susceptible to infections and
irritants in the environment.
Immune response: changes to the IgE gene, an immune
molecule, leads to the triggering of immune responses by non-harmful
environmental factors. Up to 80% of people with atopic dermatitis have
high levels of IgE.
-
The genetic change to the IgE gene is shared by all atopic
conditions (hayfever, asthma, atopic dermatitis). Should one parent have
an atopic condition, there is a 20–30% chance of their
children developing an atopic condition; this rises to 30–50% if both parents are affected.
Though individuals may have these genetic susceptibilities, they might
never develop atopic dermatitis. Similarly, some who do experience atopic
dermatitis may not have either genetic change.
Factors in the surrounding environment, known as environmental triggers,
cause atopic dermatitis to develop (or to flare up in those already
affected). Some triggers are factors associated with well-known allergies,
such as certain soaps or detergents, pollen, animal hair, clothing
materials, peanuts, or other food allergens. Other factors can include
illness, stress, dry skin, or environmental bacteria and viruses.
The particular factor, or combination of factors, that affect an
individual, can be very different from the factors that affect someone
else.